Learn More About WM
What Is Waldenstrom macroglobulinemia?
Waldenstrom macroglobulinemia (WM) is a rare, slow-growing cancer of the lymphatic system. Cancers of the lymphatic system are called lymphomas. WM is a type of lymphoma called non-Hodgkin lymphoma. Non-Hodgkin lymphoma is not a single disease; it refers to a group of different lymphomas that start in the lymphocytes (white blood cells). WM affects a specific type of white blood cell, called a B-lymphocyte or B-cell for short.
To understand WM, it’s helpful to know some basic information about your body’s lymphatic system and the function of lymphoid tissue.
What is the lymphatic system?
The lymphatic system is made up of a large network of vessels, organs, and tissues that help your body fight disease and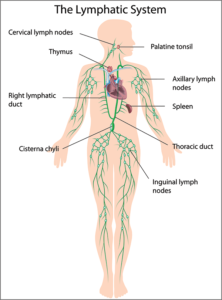 infection. Lymphoid tissue can be found in many places in the body, including:
infection. Lymphoid tissue can be found in many places in the body, including:
- Lymph nodes – small, bean-shaped glands located throughout your body. Some are found in clusters in places like your underarm area, the sides of your neck, your groin, abdomen, and chest.
- Certain organs – such as your spleen, tonsils, adenoids, and thymus.
- Bone marrow – the soft, spongy tissue in the center of most bones. This is where new blood cells are made. There are three types of blood cells:
- Red blood cells, called erythrocytes, carry oxygen throughout the body.
- Platelets, called thrombocytes, initiate the formation of blood clots to stop bleeding and help with wound healing.
- White blood cells, called lymphocytes, help the body fight infection and some diseases.
Lymphoid tissue is made mostly of white blood cells, or lymphocytes. There are two types of lymphocytes: B-lymphocytes (B-cells) and T-lymphocytes (T-cells). Normally, B-cells help your body fight infection by maturing into plasma cells. It’s the job of plasma cells to make antibodies – also called immunoglobulins or Ig for short – the proteins that help your body protect itself against infection and other types of threats. There are five main types of antibodies.
How does Waldenstrom macroglobulinemia affect the lymphatic system?
WM is a lymphoma that starts in your B-cells. When a person has WM, there has been a change, or mutation, to their B-cells resulting in the production of an abnormal lymphocyte-plasma hybrid, called a lymphoplasmacytic cell. These abnormal cancer cells multiply over and over again, and can overwhelm the bone marrow leading to a shortage of healthy blood cells in your body.
In WM, these cancer cells make abnormally large amounts of a specific antibody, called IgM. IgM is the largest of all the antibodies, called a macroglobulin. Usually, people have very low levels of IgM in their blood at any given time. With WM, you get high levels of IgM in your blood. Because of IgM’s large size and bulky structure the blood can become very thick, a condition called hyperviscosity. Thick, or viscous blood, cannot flow easily through the body. This can lead to many of the symptoms associated with WM, including excess bleeding, vision problems, cardiovascular complications, and nervous system issues.
What type of lymphoma is Waldenstrom macroglobulinemia?
WM is the most common form of a sub-type of non-Hodgkin lymphoma called lymphoplasmacytic lymphoma (LPL). WM cells are lymphoplasmacytic, meaning they have features of both plasma cells and lymphocyte cells.
WM is a slow-growing lymphoma and does not always require treatment. If you don’t have symptoms, you usually do not need to be treated. If you do develop symptoms, you may need treatment depending on the severity of the symptoms.
Learn the symptoms of WM and discuss any changes with your doctor. While there is no cure for WM yet, there are different types of treatments that can lessen or resolve your symptoms and control the disease for many years.
What are the risk factors for Waldenstrom macroglobulinemia?
A risk factor is anything that increases your chance of developing a disease. You are at higher risk for developing Waldenstrom macroglobulinemia (WM) if you:
- Are male: WM is more common in men than women.
- Are White: Caucasians are significantly more likely to develop WM than African Americans.
- Are older: There are a few cases of WM occurring in younger people, but the chance of developing this disease increases as you age. WM is most often diagnosed in adults age 65 years and older.
- Have a condition called IgM monoclonal gammopathy of undetermined significance (called IgM MGUS): This is a condition in which you have higher than normal levels of the antibody IgM – detected from blood tests – but no evidence of lymphoma.
- Have a closely-related family member with WM or another type of lymphoma.
- Have certain autoimmune diseases like Sjogren’s syndrome, or a viral illness such as hepatitis C. However, the relative importance of these factors has been difficult to determine.
How common is Waldenstrom macroglobulinemia?
WM is a rare disease. About 1,000 to 1,500 people are diagnosed with WM each year in the United States. WM accounts for approximately 1 to 2 percent of all blood (hematologic) cancers.
What causes Waldenstrom macroglobulinemia?
It’s not clear what causes WM. Experts think that changes – or mutations – in the genes of a B-lymphocyte cell is how the disease begins. These mutations tell the abnormal B-cell to continue to multiply uncontrollably. And because cancer cells don’t mature and then die as normal cells do, they accumulate and can overwhelm the production of healthy blood cells.
Recent research has identified two genetic mutations that may be found in people with WM.
- MYD88 mutation: Most people with WM (about 90 percent) have an abnormal – or mutated – version of a gene known as MYD88.
- CXCR4 mutations: Up to four out of 10 people with WM have changes to the gene known as CXCR4.
Researchers are studying what causes these genetic changes. They know they are not passed down from your parents. Most of the time, the mutations occur later in life which may explain why WM is usually diagnosed in older people. It’s likely these mutations do not cause WM by themselves, but in combination with other factors.


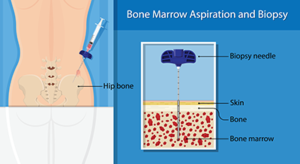 confirmed by testing your bone marrow. The bone marrow samples are sent to a laboratory to be examined by an expert in diagnosing diseases of the bone marrow and blood, called a hematopathologist. He or she will look for the lymphoplasmacytic cells of WM, which have features of both B-lymphocytes and plasma cells.
confirmed by testing your bone marrow. The bone marrow samples are sent to a laboratory to be examined by an expert in diagnosing diseases of the bone marrow and blood, called a hematopathologist. He or she will look for the lymphoplasmacytic cells of WM, which have features of both B-lymphocytes and plasma cells. body. They are not needed to diagnose WM; however, they help your doctor determine whether the cancer has spread beyond your bone marrow to other parts of your body.
body. They are not needed to diagnose WM; however, they help your doctor determine whether the cancer has spread beyond your bone marrow to other parts of your body.